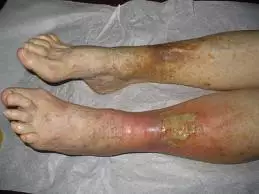
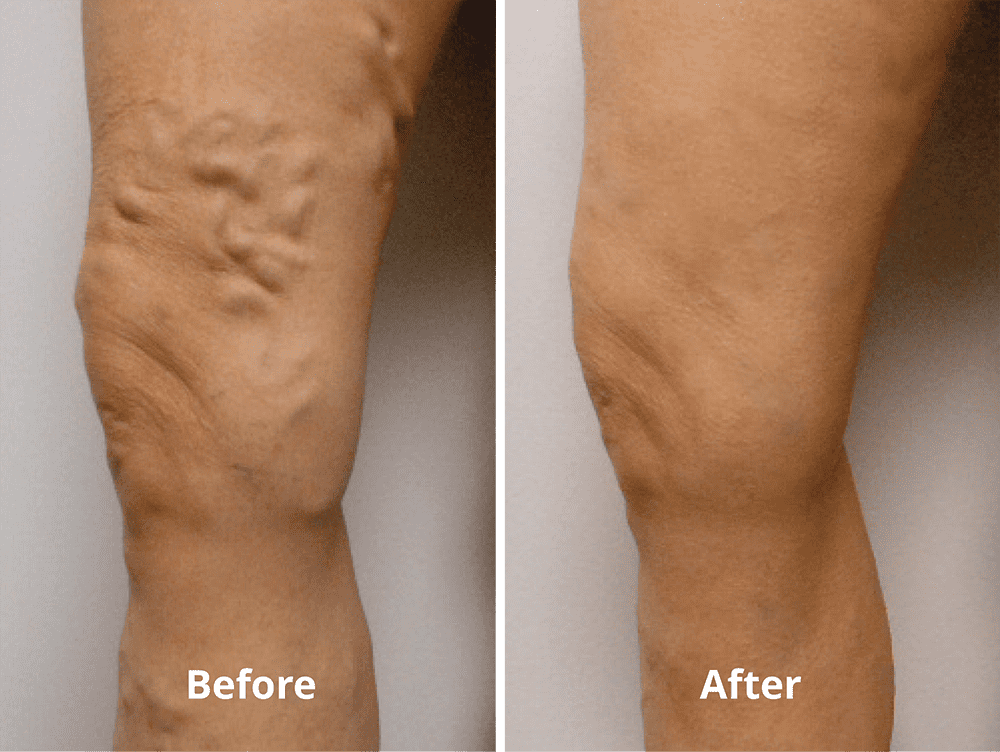
A venous ulcer, also called a stasis ulcer, is a shallow wound that usually develops on the legs as a result of advanced vein disease. Venous ulcers are common in patients who have a history of leg swelling, varicose veins, venous insufficiency, certain health conditions or blood clots in either the superficial or deep veins of the legs. Venous ulcers affect over 500,000 people in the United States every year and account for approximately 80 percent of all leg ulcers.
What Causes a Venous Ulcer?
Vein disease is the root cause of a venous ulcer. Vein disease develops when the one-way valves inside of a vein stop functioning correctly. The one-way valves are designed to push blood toward the heart; however, sometimes the valves weaken and are unable to adequately return the blood to the heart. As a result, excess blood remains in the vein, which creates increased pressure on the vein wall. Further, the excess blood has nowhere to go, so it pools in the lower extremities. The pooled blood may seep out of the vein and into surrounding tissue, causing the skin to become discolored and tender. If left untreated, the excess blood and pressure can break down the skin from the inside out and create open, painful sores on the surface of the skin. Once a venous ulcer has developed, it can be challenging to treat and can take weeks, months or even years to heal.